Types Of Colon Polyps
Colon polyps are growths that occur on the inner lining of the colon or rectum. They are quite common, and most people who have them do not experience any symptoms. However, some types of polyps can become cancerous over time, which is why it is important to understand the different types of colon polyps and their associated risks.
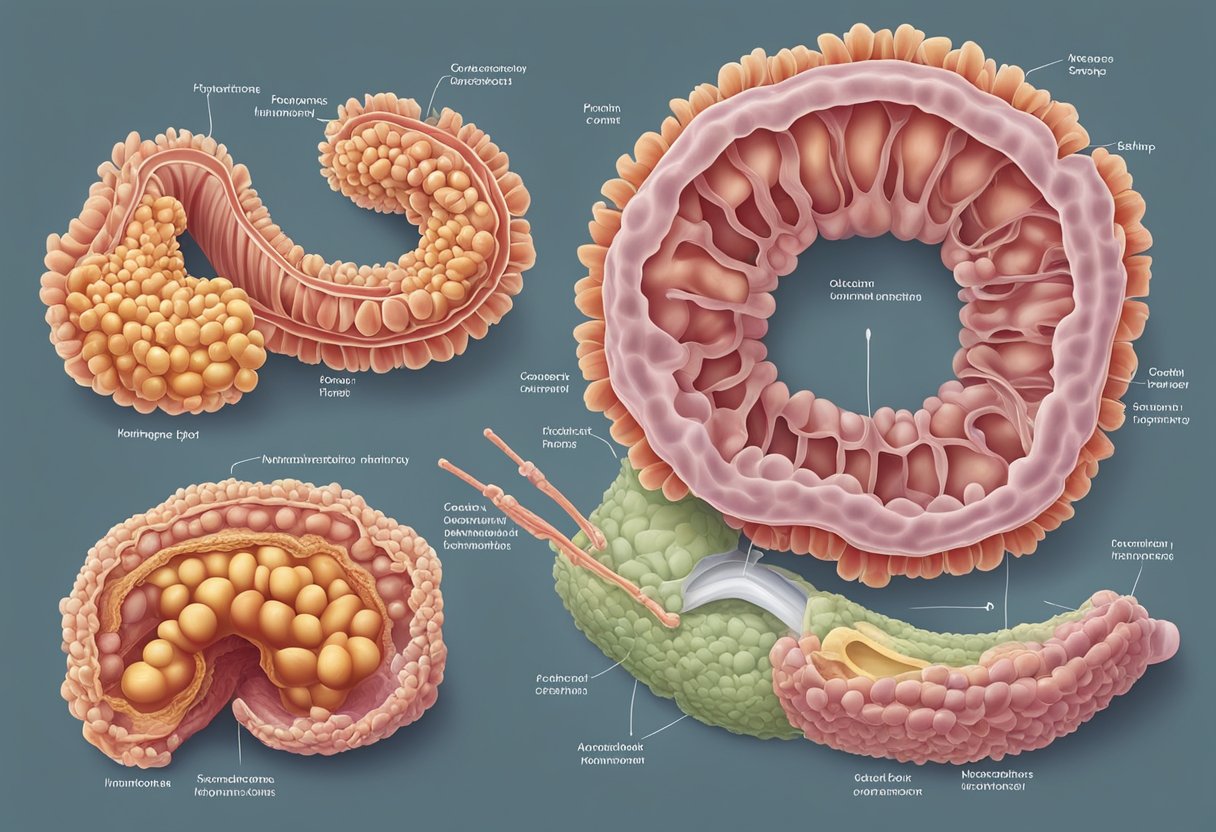
There are several different types of colon polyps, including adenomatous, hyperplastic, and serrated polyps. Adenomatous polyps are the most common, and they have the highest risk of becoming cancerous. Hyperplastic polyps are typically benign, while serrated polyps have a slightly higher risk of becoming cancerous than hyperplastic polyps. Understanding the differences between these types of polyps can help individuals and their healthcare providers make informed decisions about screening and treatment options.
Key Takeaways:
- Colon polyps are growths on the inner lining of the colon or rectum.
- There are several types of colon polyps, including adenomatous, hyperplastic, and serrated polyps.
- Adenomatous polyps have the highest risk of becoming cancerous, while hyperplastic and serrated polyps are typically benign.
Understanding Colon Polyps
Definition and Types
Colon polyps are small growths that develop on the inner lining of the colon or rectum. They are usually benign, but some types of polyps can turn into colon cancer over time. There are different types of colon polyps, including adenomatous polyps, hyperplastic polyps, inflammatory polyps, serrated polyps, neoplastic polyps, and non-neoplastic polyps.
Adenomatous polyps are the most common type of colon polyps and are considered precancerous. They can be further classified as tubular adenomas, villous adenomas, or tubulovillous adenomas based on their shape and size. Hyperplastic polyps are the second most common type of colon polyps and are usually benign. Inflammatory polyps are caused by inflammation in the colon and are also usually benign.
Serrated polyps are a group of polyps that have a saw-toothed appearance under the microscope. They can be further classified as hyperplastic polyps with serrated architecture, sessile serrated adenomas/polyps, or traditional serrated adenomas based on their features. Neoplastic polyps are a type of adenoma that has abnormal cells and can turn into cancer over time. Non-neoplastic polyps are usually benign and include juvenile polyps, inflammatory polyps, and hamartomatous polyps.
Prevalence and Incidence
Colon polyps are common, with up to 30% of adults over the age of 50 having at least one polyp. The prevalence of colon polyps increases with age, and they are more common in men than women. Some factors that increase the risk of developing colon polyps include a family history of colon cancer or polyps, a personal history of colon cancer or polyps, inflammatory bowel disease, and a diet high in red meat and low in fiber.
It is important to get regular screenings for colon polyps and colon cancer, especially if you are at a higher risk. Screening tests include colonoscopy, fecal occult blood test, and stool DNA test. Your doctor can recommend the best screening test for you based on your age, medical history, and risk factors. Early detection and removal of colon polyps can prevent colon cancer from developing or catch it at an early stage when it is more treatable.
Risk Factors and Causes
Colon polyps can develop in anyone, but certain factors can increase the risk of developing them. Here are some of the common risk factors and causes associated with colon polyps:
Genetic Predispositions
Family history plays a significant role in the development of colon polyps. People with a family history of colon polyps or colon cancer are at higher risk of developing colon polyps themselves. Inherited conditions such as familial adenomatous polyposis (FAP) and Lynch syndrome also increase the risk of developing colon polyps.
Lifestyle and Dietary Factors
Certain lifestyle and dietary factors can also contribute to the development of colon polyps. Age is a significant risk factor, as the risk of developing colon polyps increases with age. Unhealthy diets that are high in fat and low in fiber can also increase the risk of colon polyps. Smoking and excessive alcohol use have also been linked to an increased risk of colon polyps.
It is important to note that not all colon polyps are cancerous, and most people with colon polyps do not develop colon cancer. However, regular screening and early detection are essential for preventing the development of colon cancer.
Symptoms and Detection
Recognizing Symptoms
Colon polyps may not always cause symptoms, which is why regular screening is important. However, some people may experience symptoms such as:
- Rectal bleeding or blood in the stool
- Anemia (low red blood cell count)
- Abdominal pain or cramping
- Changes in bowel habits, such as diarrhea or constipation
It is important to note that these symptoms may also be caused by other conditions, such as hemorrhoids or inflammatory bowel disease. Therefore, it is important to consult a healthcare professional for an accurate diagnosis.
Screening and Diagnosis
Screening for colon polyps is typically done through a colonoscopy, which is a procedure that allows a doctor to examine the entire colon. During a colonoscopy, any polyps found can be removed and sent for biopsy to determine if they are cancerous.
Other screening tests for colon polyps include the fecal occult blood test (FOBT), virtual colonoscopy, and flexible sigmoidoscopy. These tests may be used as alternatives to colonoscopy in certain cases.
If a person is found to have colon polyps, their doctor will recommend a surveillance plan to monitor for any changes or growth in the polyps. Depending on the type and number of polyps found, the surveillance plan may include frequent colonoscopies or other tests.
Overall, early detection and removal of colon polyps is key in preventing the development of colon cancer. It is recommended that individuals at average risk for colon cancer begin screening at age 45, while those at higher risk may need to start screening earlier. Consult with a healthcare professional to determine the appropriate screening plan for you.
Treatment and Management
Non-Surgical Approaches
In most cases, colon polyps are removed during a colonoscopy. However, if the polyp is too large or located in a hard-to-reach area, non-surgical approaches may be used.
One such approach is polypectomy, which involves the removal of the polyp using a wire loop or snare. This procedure is usually done during a colonoscopy and is minimally invasive.
Another non-surgical approach is endoscopic mucosal resection (EMR), which is used for larger polyps that cannot be removed with a polypectomy. EMR involves the use of a special instrument to remove the polyp from the colon wall.
Surgical Interventions
If the polyp is too large or cancerous, surgical intervention may be necessary. A surgeon will remove the affected portion of the colon, along with any nearby lymph nodes that may be affected.
After surgery, patients will need to follow up with their healthcare provider regularly to monitor for recurrence of polyps or cancer.
It is important for individuals to follow a healthy lifestyle to help lower their chances of developing colon polyps. This includes regular physical activity, avoiding smoking and excessive alcohol consumption, and maintaining a healthy weight.
In summary, treatment and management of colon polyps may involve non-surgical approaches such as polypectomy and EMR, or surgical intervention if the polyp is too large or cancerous. Maintaining a healthy lifestyle is also important in preventing the development of colon polyps.
Prevention and Long-Term Outlook
Colon polyps are a common condition that can lead to colon cancer if left untreated. Fortunately, there are steps individuals can take to prevent the development of colon polyps and reduce their risk of colon cancer. In this section, we will discuss lifestyle modifications and regular screening and surveillance as two key ways to prevent and manage colon polyps.
Lifestyle Modifications
One of the most effective ways to prevent colon polyps is to make lifestyle modifications. Individuals can reduce their risk of developing colon polyps by:
- Eating a diet that is high in fiber and low in fat
- Exercising regularly
- Maintaining a healthy weight
- Avoiding smoking and excessive alcohol consumption
By making these lifestyle changes, individuals can reduce their risk of developing colon polyps and improve their overall health.
Regular Screening and Surveillance
Another important way to prevent colon polyps is through regular screening and surveillance. Screening tests can detect colon polyps before they become cancerous, allowing for early intervention and treatment. The American Cancer Society recommends that individuals at average risk of colon cancer begin regular colon cancer screening at age 45. Individuals at high risk of colon cancer may need to begin screening earlier or undergo more frequent screening.
Colon cancer screening tests include:
- Colonoscopy
- Fecal immunochemical test (FIT)
- Stool DNA test
The frequency of colon cancer screening tests depends on an individual’s risk factors. For individuals at average risk, colon cancer screening tests should be performed every 10 years. Individuals at high risk may need to undergo more frequent screening.
In conclusion, lifestyle modifications and regular screening and surveillance are two key ways to prevent and manage colon polyps. By making these changes and undergoing regular screening tests, individuals can reduce their risk of developing colon polyps and colon cancer.